Survivor Views on Rural Health
Overview
The American Cancer Society Cancer Action Network (ACS CAN) empowers advocates across the country to make their voices heard and influence evidence-based public policy change, as well as legislative and regulatory solutions that will reduce the cancer burden. As part of this effort, ACS CAN deploys surveys to better understand cancer patient and survivor experiences and perspectives, through our Survivor Views research panel. The panel is a group of cancer patients and survivors who respond to regular surveys and provide important insights to support ACS CAN’s advocacy work at all levels of government.
Fielded March 17-April 7, 2026, our latest survey explores the experiences of cancer patients and survivors in rural communities. The web-based survey was conducted among 1,436n cancer patients and survivors nationwide, including 483n residing in rural communities, who have been diagnosed with or treated for cancer in the last seven years. More methodological detail follows at the end of this report.
Key Findings
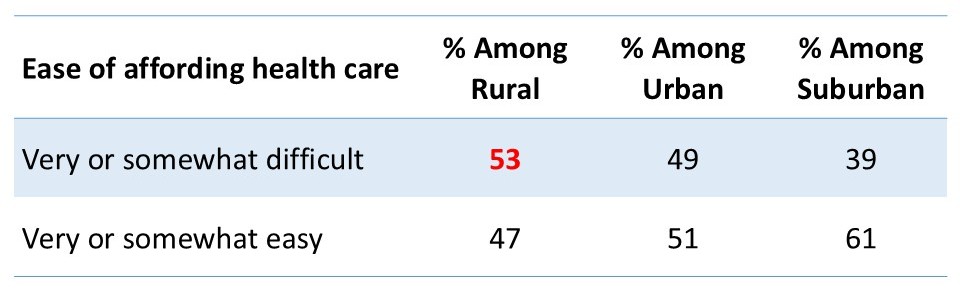
- Cancer patients and survivors in rural areas are significantly more likely than those in other areas to find it difficult to afford their health care (53%).
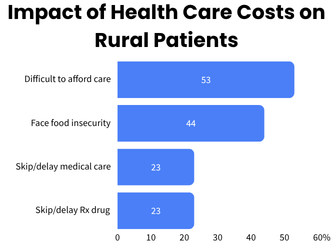
- They are more likely to have incurred medical debt related to the costs of their cancer care (50%) and are more worried about incurring new medical debt as a result of their cancer care (70%).
- As a result of these additional cost burdens, rural cancer patients and survivors are more likely to skip or delay recommended medical care (23%), skip or delay taking a prescribed medication (23%), and face food insecurity (44%).
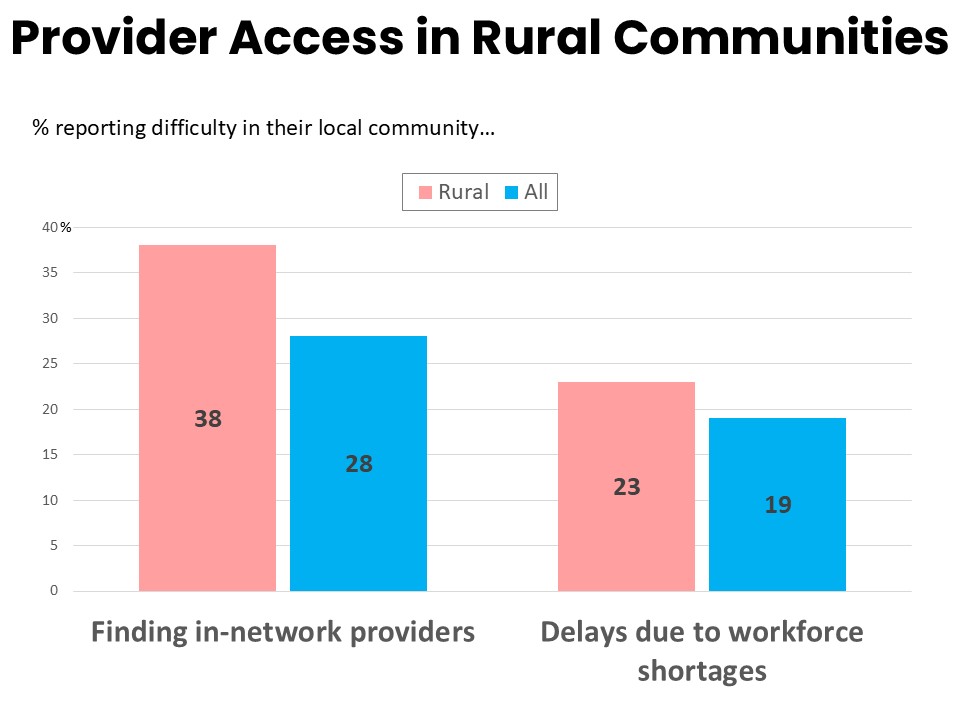
- Rural cancer patients and survivors report greater difficulty finding in-network providers in their area (38% say this is difficult) and are more likely to report difficulty and delays related to health care provider workforce shortages (23%).
- Traveling long distances to specialists can be especially difficult (45%). Over a third (37%) of rural cancer patients and survivors travel more than an hour to reach their primary oncology provider, and 34% have had to travel far enough from their community that they and/or their caregiver had to sleep away from home during treatment.
- Rural respondents also lag in keeping their cancer screenings up-to-date and face additional barriers to accessing any needed follow up resulting from their screening (27%).
- While rural patients rate the quality of the care they received in their local community below residents in other areas, those who receive patient navigation services report reduced barriers to care and improved quality of care.
Detailed Survey Findings
Rural Cancer Patients and Survivors Report Significant Difficulty Affording Care
Over half (53%) of cancer patients and survivors residing in rural communities report that it has been very or somewhat difficult to afford their health care. Forty-four percent say the cost of their cancer care has at some point affected their ability to afford purchasing food. Nearly a quarter (23%) have skipped or delayed recommended medical care due to concerns about the costs and the same number have skipped or delayed taking a prescribed medication due to difficulty paying for prescription drugs. One-in-ten say the expected cost is the most important factor in their decision when a provider recommends a treatment, procedure, test, or other service while another 35% say cost is one of the factors they consider.
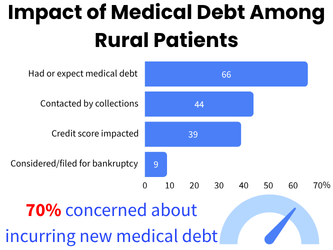
Half of rural survey respondents (50%) report having incurred medical debt due to the costs of their cancer care, and another 16% who are just beginning treatment expect to accumulate medical debt as a result. Forty-four percent have been contacted by a collections agency about debt related to their cancer care and 39% say their credit score has been impacted by their cancer-related debt. Nine percent have filed or considered filing for bankruptcy due to the costs of their cancer care. An overwhelming majority (70%) are concerned about incurring new debt as a result of the costs related to their cancer care.
Workforce and Network Adequacy Concerns Add to Travel Time and Costs
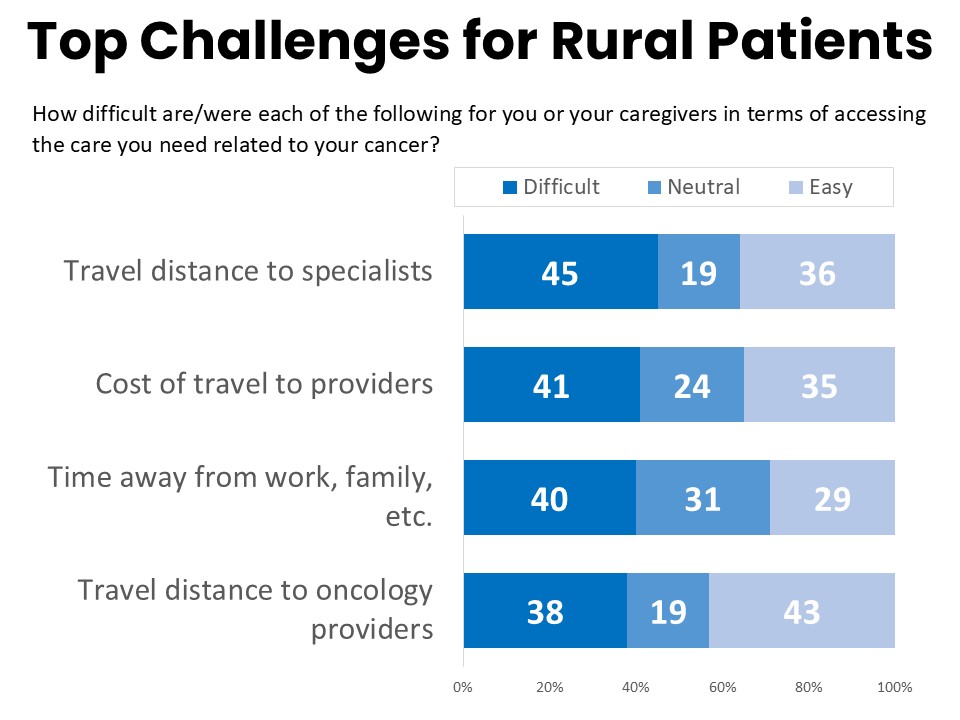
Thirty-eight percent of rural respondents report that it is difficult to find providers within their health care network in the area where they live, a rate ten percentage points higher than patients nationwide. Nearly a quarter (23%) have faced difficulty or delays in accessing care due to workforce shortages of health care professionals in their area. Travel distance to the specialists or specialized services many cancer patients require was rated most difficult among a list of challenges (45% difficult). Costs of travel to providers (41%) and time away from work, family, or other responsibilities (40%) rank next in terms of difficulty, followed by travel distance to oncology providers (38%).
Over a third (37%) of rural cancer patients and survivors travel more than an hour to reach their primary oncology provider, and 34% have had to travel far enough from their community that they and/or their caregiver had to sleep away from home during treatment. The majority of those (61%) paid for their hotel or housing themselves. One-in-five have worried that the amount of travel time required for their cancer care might cause them to lose their job and/or risk the health care coverage they relied upon for care. This number jumps to 35% when excluding those who were not working at the time of their cancer treatment.
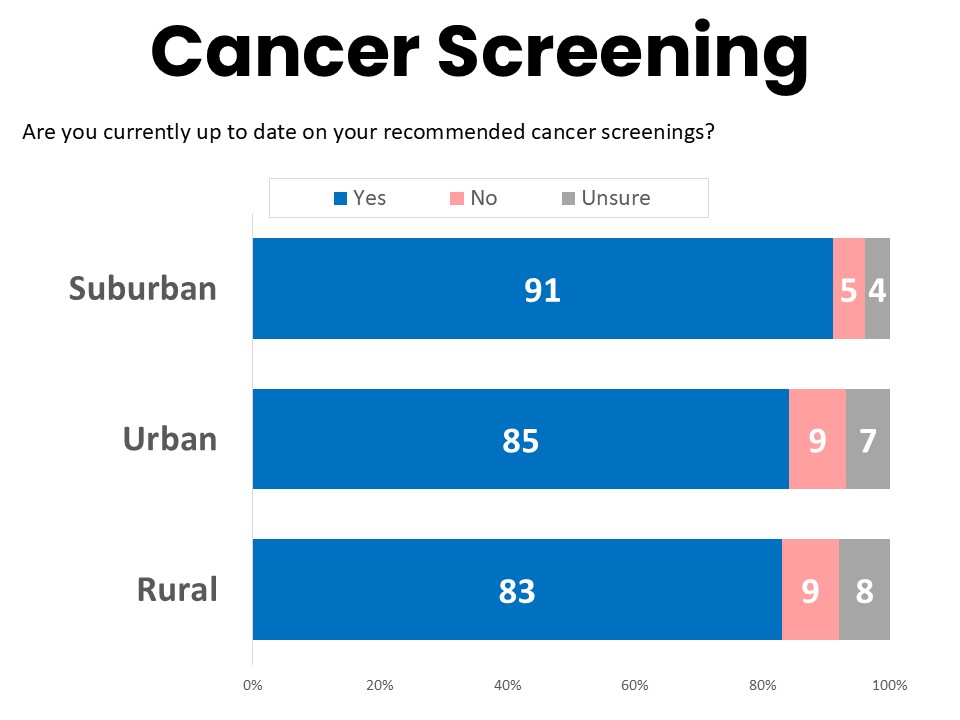
Rural Cancer Patients and Survivors Lag in Screening and Face Barriers to Accessing Follow Up Care
The challenges for rural patients described above start even before they are diagnosed, creating barriers to early detection and prevention. Our survey finds cancer patients and survivors in rural areas are less likely than others to be up to date on recommended cancer screenings, with 83% in rural areas up to date compared to 91% in suburban areas.
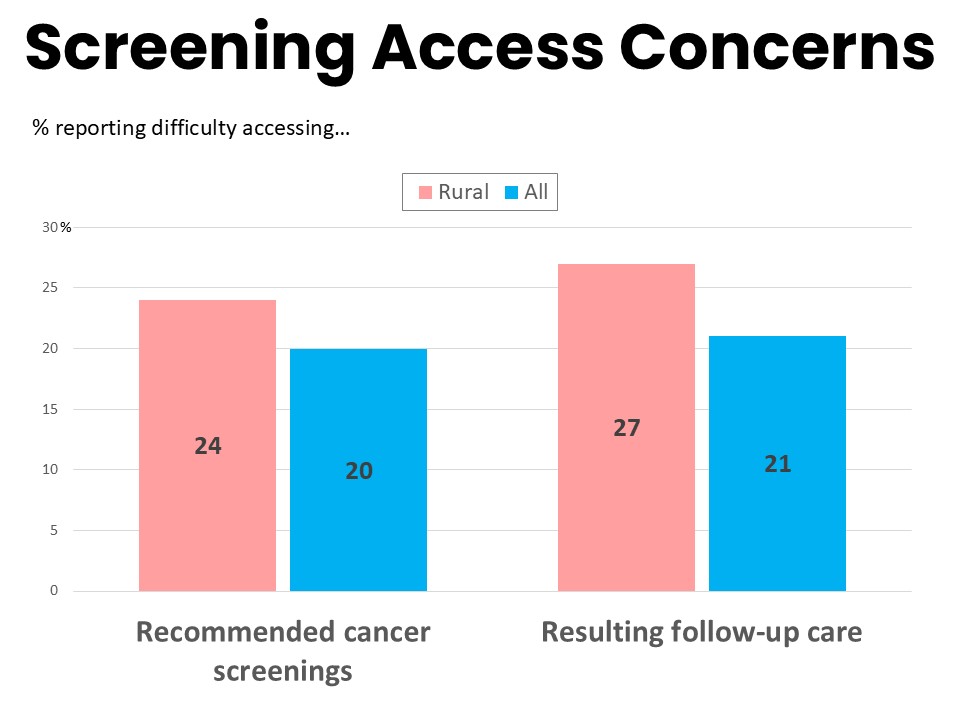
Rural patients and survivors are more likely to report difficulty accessing recommended cancer screenings, with 24% of rural respondents reporting this difficulty compared to 20% nationwide and 16% of suburban residents. They are also significantly more likely to report difficulty accessing any follow up care resulting from those screenings: 27% in rural areas find it difficult to access follow up care compared to 21% nationally and 17% in suburban communities. Rural respondents are also less likely to see a primary care doctor annually for well visits (74% of rural respondents vs. 81% suburban) and more likely to see their doctor only as needed for illness or required visits (22% of rural respondents vs. 15% suburban). Three-in-ten say their provider does not talk to them about cancer prevention and/or early detection, such as recommended cancer screenings, tobacco cessation, or proper nutrition.
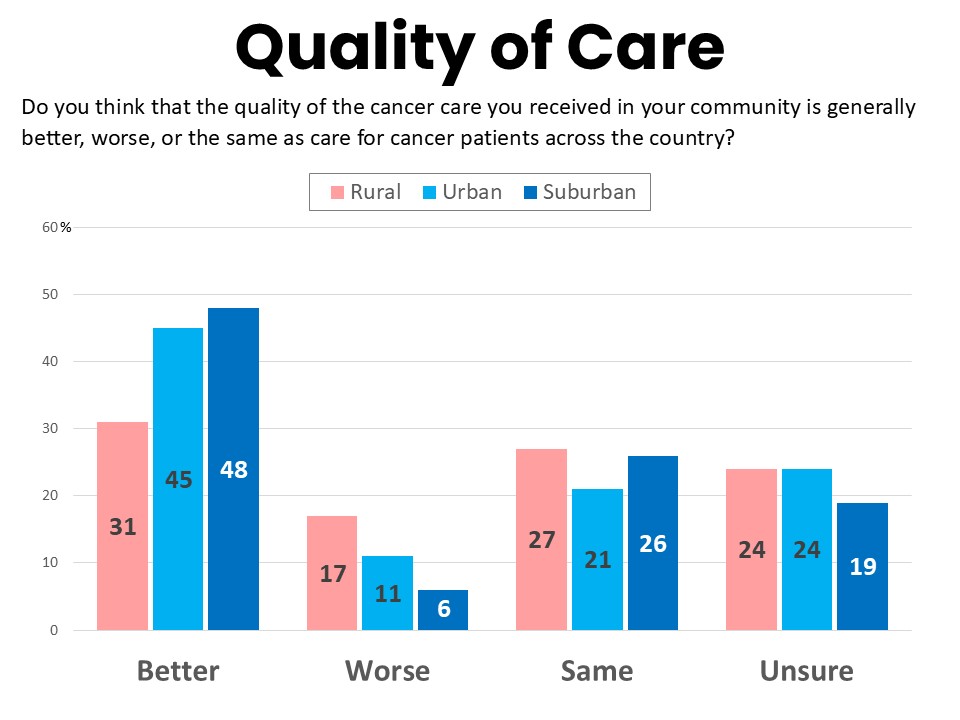
Quality Concerns and Barriers to Care Can Be Offset by Patient Navigation
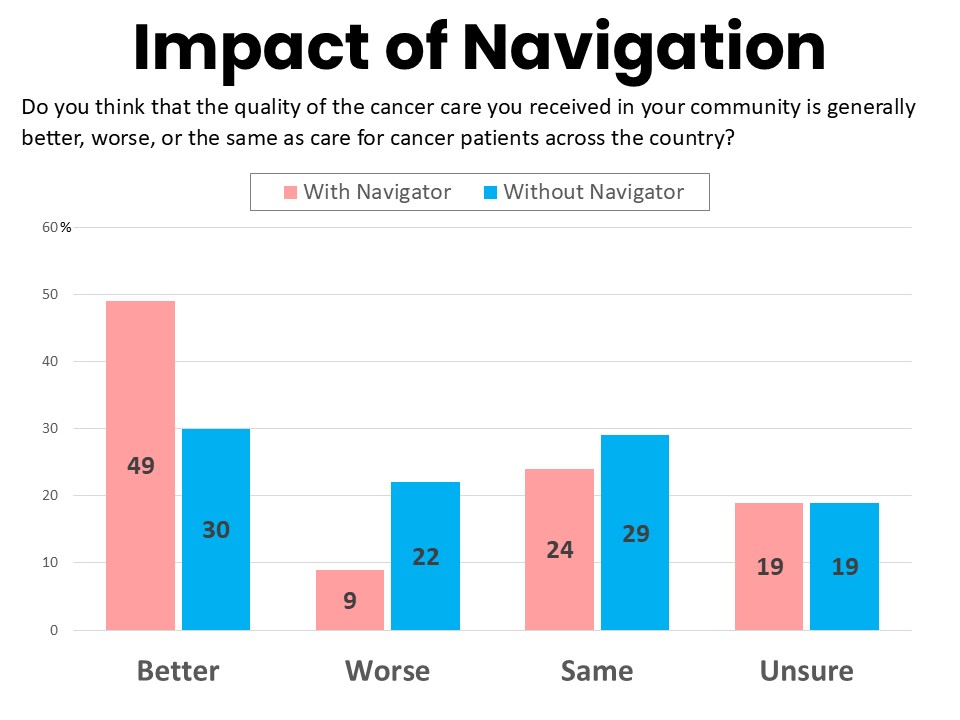
Rural residents generally report positively about the quality of health care in their area with 74% rating it excellent or good compared to 26% rating it fair or poor. However this is significantly lower than the 88% of suburban residents who consider the quality of their local care to be excellent or good. Furthermore, while 31% of rural respondents believe the quality of care in their community is generally better than care for cancer patients across the country, significantly higher percentages of suburban residents (48%) and urban residents (45%) feel this way. Rural residents are significantly more likely than others to believe the quality of care they received in their community is worse than for cancer patients across the country (17%).
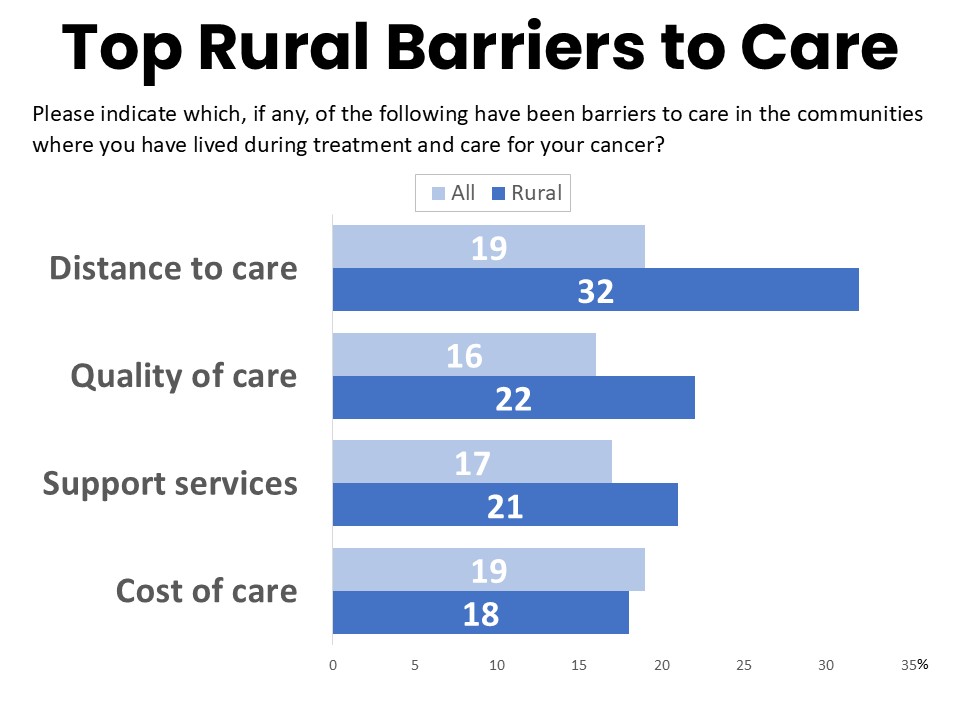
Distance to care and services in the local area is the most frequently cited barrier to care for rural residents (32% say this is a barrier), followed by the quality of care and services in the local area (22%) and a lack of support resources (21%), such as assistance with transportation or lodging, mental health services, support groups, or access to social workers.
However, 51% of rural patients and survivors report that their primary oncology provider has a dedicated patient navigator on staff. Patient navigators offer individualized assistance to patients, families, and caregivers to help overcome health care system barriers and facilitate timely access to quality care. Those with access to a patient navigator were less likely to rate all of the above issues as barriers and more likely to rate their quality of care highly. For example, among those with access to a patient navigator, 49% feel the quality of care in their community is generally better than care for patients across the country.
Methodology
ACS CAN’s Survivor Views research initiative was designed to support the organization’s efforts to end suffering and death from cancer through public policy advocacy. Data provided by cancer patients and survivors as part of this project allows for a greater understanding of their experiences and opinions on cancer-related issues and gives voice to cancer patients and survivors in the shaping and advocating of public policies that help prevent, detect, and treat cancer and promote a more positive quality of life for those impacted.
To ensure the protection of all participants in this initiative, all research protocols, questionnaires, and communications are reviewed by the Morehouse School of Medicine Institutional Review Board.
The survey population is comprised of individuals who meet the following criteria:
- Diagnosed with and/or treated for cancer within the last seven years
- Over the age of 18 (parents of childhood cancer survivors were invited to participate on behalf of their minor children)
- Reside in the US or US territories
Survivor Views participants are invited to participate through email, direct mail, social media, and outreach to communities and partners engaged with cancer patients and survivors. Those who agree to participate after reviewing the informed consent information are invited to join the Survivor Views research cohort and participate in future surveys.
The data for this survey were collected between March 17-April 7, 2026. A total of 1,436 participants responded to the survey. Respondents self-identified as rural, urban, or suburban based on their perception of the community where they live using the standard survey question used by Pew Research Center and others. As Pew researchers have stated, “Classifications for whether a given area is urban, suburban or rural are inherently subjective, which is one of the main reasons we have typically relied on self-reported information at Pew Research Center.”
About ACS CAN
The American Cancer Society Cancer Action Network (ACS CAN) advocates for evidence-based public policies to reduce the cancer burden for everyone. We engage our volunteers across the country to make their voices heard by policymakers at every level of government. We believe everyone should have a fair and just opportunity to prevent, detect, treat, and survive cancer. Since 2001, as the American Cancer Society’s nonprofit, nonpartisan advocacy affiliate, ACS CAN has successfully advocated for billions of dollars in cancer research funding, expanded access to quality affordable health care, and advanced proven tobacco control measures. We stand with our volunteers, working to make cancer a top priority for policymakers in cities, states and our nation’s capital. Join the fight by visiting www.fightcancer.org.