Overview:
The American Cancer Society Cancer Action Network (ACS CAN) gives voice to cancer patients and survivors on critical public policy issues that affect their lives. As part of this effort, ACS CAN deploys surveys to better understand cancer patient and survivor experiences and perspectives, through our Survivor Views research panel. The panel is a group of cancer patients and survivors who respond to regular surveys and provide important insights to support ACS CAN’s advocacy work at all levels of government.
Fielded May 16-26, 2022, the latest survey explores cancer patients’ and survivors’ experiences and perspectives on copay assistance, patient navigation, and digital therapeutics. The web-based survey was conducted among 1,241 patients and survivors nationwide diagnosed with or treated for cancer in the last seven years, along with oversamples of 1,370 targeted interviews (see methodological note at end). The margin of sampling error associated with a sample of this size is +/-2.8% at a 95% confidence level.
Key Findings:
- Cancer care is expensive and prescription drug costs are a challenge for nearly one-third of cancer patients and survivors (31%), with one-fifth having skipped or delayed taking prescribed medications due to costs. The number of patients who have skipped or delayed treatment because of costs is higher among Black, Hispanic, Asian, and lower income patients.
- About half have heard of copay assistance programs but just one-quarter have applied to one. Those who have enrolled agree that the assistance provides access to medication through the program that they otherwise couldn’t afford (83%), while some who were unable to enroll reported declining treatment (8%) or going into debt to cover their prescription drug costs (18%).
- These negative impacts are even greater among some patient populations, with over one-quarter of Black, Hispanic, and Asian cancer patients and survivors reporting they have declined treatment due to cost after finding they were unable to enroll in a copay assistance program.
- The most difficult tasks for cancer patients and survivors tend to be those they are less likely to report receiving support for, with emotional support such as for feeling overwhelmed or dealing with fears rating as the most difficult aspect of care among those tested.
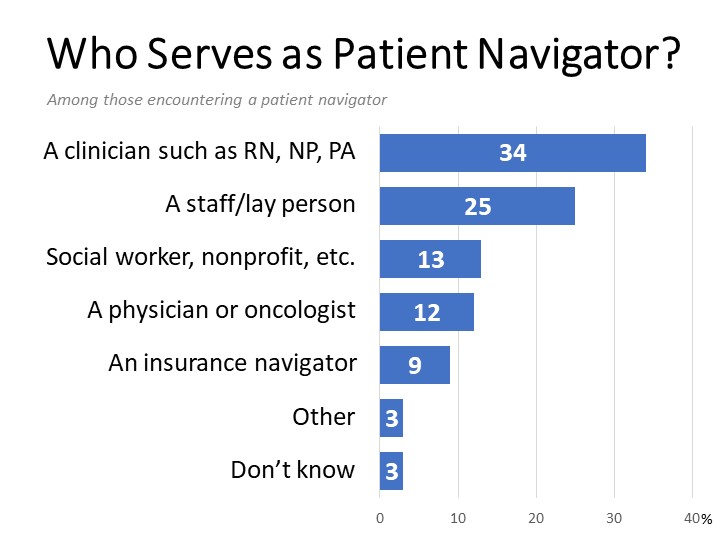
- Just over half have encountered someone fulfilling the role of a patient navigator, though definitions and tasks associated with the role vary. Clinical staff such as nurses, nurse practitioners, physician assistants, and nurse navigators are most often associated with the role of patient navigator.
- A strong majority (79%) agree that having a single contact for the issues addressed by patient navigators is very important for cancer patients.
- Sixty-three percent of cancer patients and survivors would be likely to use digital therapeutics prescribed by their physician, however a quarter are unsure with concerns including clarity about the benefits, associated costs, and privacy.
Detailed Survey Findings:
Prescription Drug Costs are a Challenge for Nearly a Third of Cancer Patients and Survivors
Thirty-one percent of cancer patients and survivors find it difficult to afford their prescription drug costs. Among patients with annual household income below $35,000, 45% find prescription drug costs difficult and one-in-five say it is very difficult to afford them. One-fifth report having skipped or delayed taking a prescribed medication due to difficulty paying the cost, with significantly higher rates of missed medication reported by lower income (44%), Asian/Pacific Islander (40%), Black (44%), and Hispanic (58%) patients and survivors.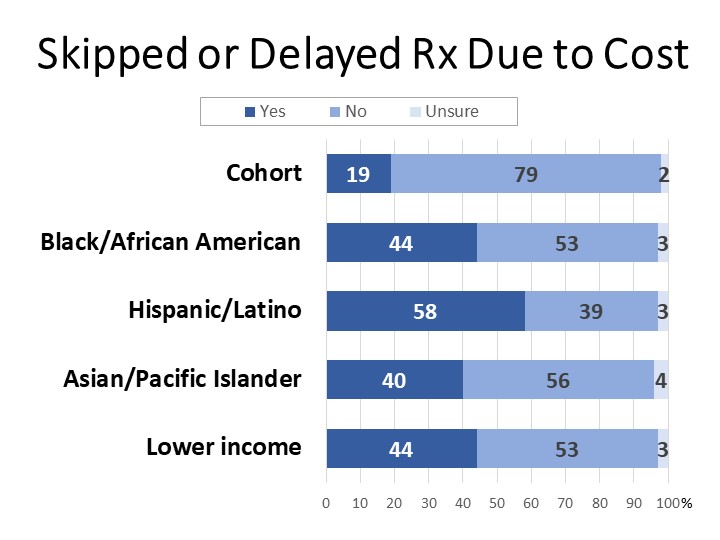
Copay Assistance Programs Help Ensure Patients Receive Needed Medications
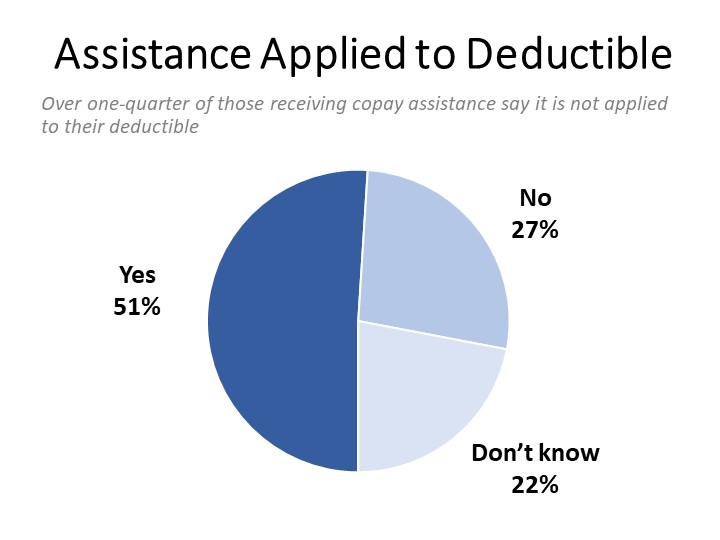
Although 51% have heard of copay assistance programs, most have not tried to enroll: 20% have applied and enrolled while 5% report applying but not ultimately enrolling. Over a quarter (27%) of those who enrolled report that the assistance they received was not applied to their deductible or other out-of-pocket cost requirements and another 22% were unsure. Among those who were unable to enroll in a copay assistance program they applied to, 18% ultimately borrowed money or went into debt to cover their prescription drug copayment costs while 15% declined the treatment (8%) or sought a less expensive treatment than their doctor had prescribed (7%).
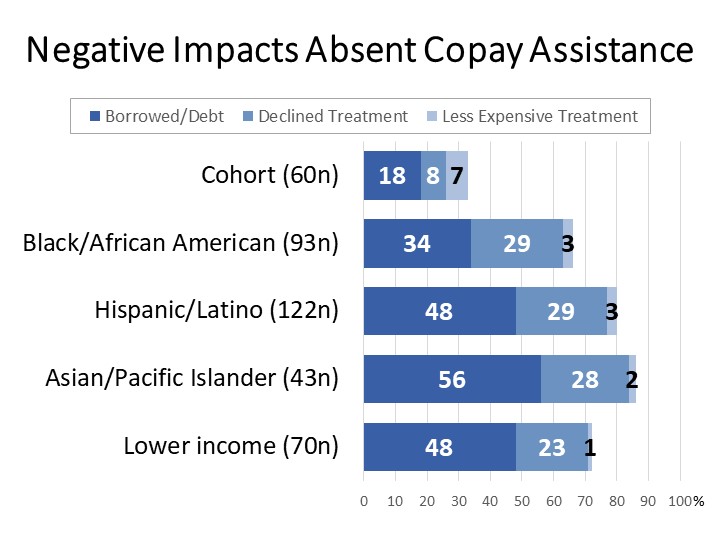
For some populations, the negative impacts of not being able to enroll in copay assistance programs are more pronounced. Over a quarter of Black (29%), Hispanic (29%), and Asian (28%) patients and survivors reported declining the treatment due to cost after being unable to enroll in a copay assistance program, along with 23% of lower income respondents. These groups report even higher rates of borrowing money or accumulating debt in order to cover the costs of their prescription drugs after finding they were unable to enroll upon applying to a program.
Among cancer patients and survivors who have enrolled in copay assistance programs, the benefits are clear. Eighty-five percent agree that the assistance they receive provides significant savings, making their prescription drug costs much more affordable, while 83% say it helps them access medication they otherwise could not afford, and allows them to take their medication as prescribed. While 78% agree the copay assistance program they used was simple and easy to understand (41% strongly agree), 97% say it is important for programs like copay assistance to be as simple and easy to use as possible for cancer patients (92% strongly agree).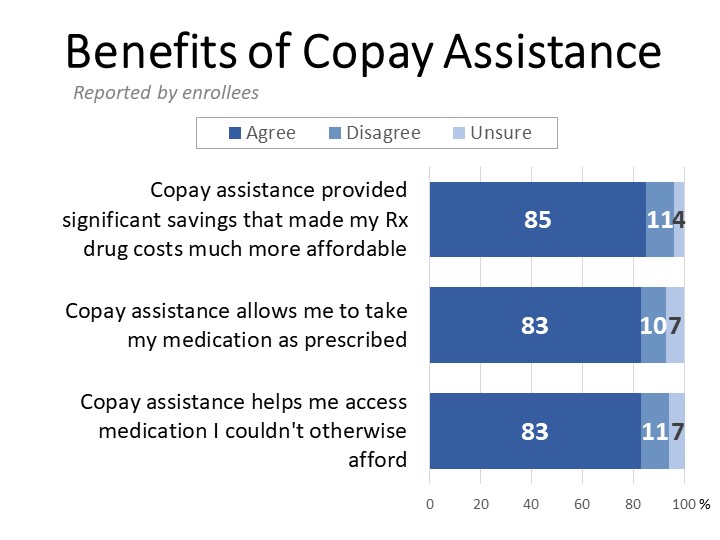
Just Over Half Have Encountered a Patient Navigator During Cancer Care
The term “patient navigator” is familiar to just over half (53%) of cancer patients and survivors surveyed, with about the same number (54%) having encountered a person who fulfills the role of patient navigator as defined in the survey. For this survey, a patient navigator was defined as follows:
“Patient navigators help guide patients through the often-complicated health care system with the resources they need to get care. A patient navigator helps patients communicate with their healthcare providers so they get the information they need to make decisions about their health care. Patient navigators may also help patients set up appointments for doctor visits and medical tests and get financial, legal, and social support.”
Among the 54% who have encountered someone fitting this description, most report a member of their provider’s clinical staff such as a nurse, nurse practitioner, physician assistant, or nurse navigator (34%) serving as a patient navigator. Another 25% say a lay person trained as a patient navigator fulfilled this role, which equates to 12% of the total sample having encountered a dedicated staff layperson serving as a patient navigator, and 29% who have had a clinical or lay person serve as patient navigator. Thirteen percent cited a social worker, community service, case manager, non-profit or other entity outside of their provider’s practice fulfilling the navigator role, while 12% said their doctor or oncologist best fit the patient navigator description. Nine percent encountered an insurance navigator or coordinator affiliated with their insurance coverage who fulfilled the role of a patient navigator.
Patient navigators may assist with a wide range of tasks. The table below shows the tasks measured in this survey, sorted by those cancer patients have the most difficulty with, along with the percentage reporting who, if anyone, provided support with these tasks:
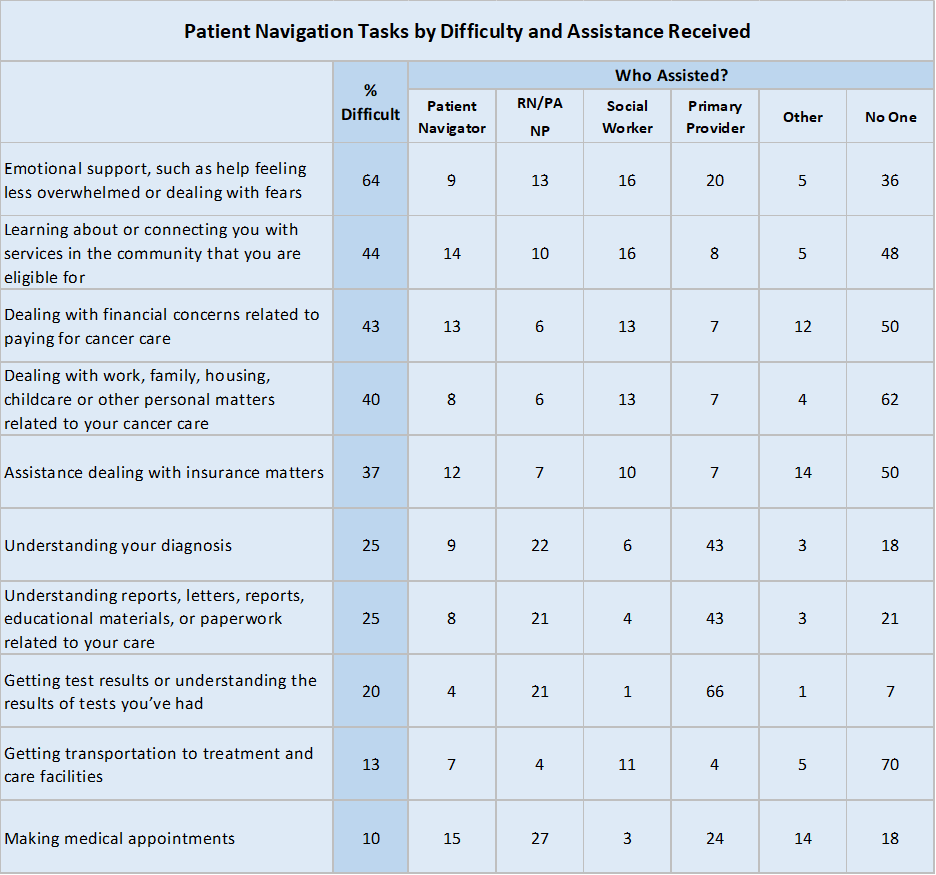
The most difficult tasks for cancer patients and survivors are typically those for which they have not received support. Making medical appointments, for example, is the most frequently associated task done by a patient navigator and/or otherwise well supported, and also garners the lowest difficulty rating of the tasks measured (10% say this is difficult). Emotional support (64% difficult), connecting with community services (44% difficult), dealing with financial or insurance concerns (43% and 37% difficult, respectively), and dealing with personal matters such as work, family, and housing (40% difficult) are the most difficult for cancer patients and survivors, and are among those least likely to be associated with receiving support (ranging from 36% to 62% saying they did not receive support in these areas). The exception is transportation, which 70% did not receive support for but also was not seen as difficult by this population (13% difficult).
After making medical appointments (15%), the tasks most frequently associated with patient navigators are connecting patients with services for which they may be eligible (14%), dealing with financial concerns related to paying for care (13%), and assistance with insurance matters (12%). Getting or understanding test results (66%), understanding diagnoses (43%), and understanding reports or additional information related to care are tasks that are most associated with the primary provider responsible for the patient’s cancer care. Providers are meanwhile also the most frequently mentioned role associated with patients’ most difficult issue: emotional support such as help feeling less overwhelmed or dealing with fears (20% received support from provider); however, with a range of sources providing emotional support, a total of 64% of cancer patients and survivors report receiving some emotional support.
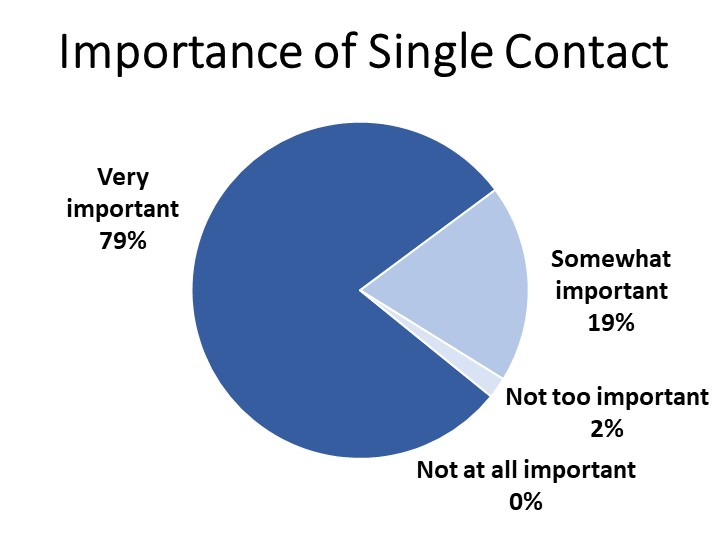
While definitions and experiences with patient navigators vary, cancer patients and survivors widely agree that having access to a single point of contact who can help them get information they need, help set up appointments for doctor visits and medical tests, and help patients get financial, legal, and/or social support is very important. Comments from cancer patients and survivors shed light on why the patient navigator role is so important:
“When you're going through treatment, it's hard to deal with the present while also looking around for the help you need.”
“It felt like everyone just assumed I knew what was going on and that I knew how to reach out for help. They seemed surprised when I asked questions and said things like, "They haven't reached out to you yet?" They never said who “they” were, just that they would have whomever it was reach out to me. Most of the time I never knew if they did or not.”
“During the first week after my diagnosis, while I was hospitalized, there were many nurses who provided excellent care, but not someone to help me understand what was happening and guide me toward the "next steps." One person, with a face and a name, to assist me during that first week and be available after I was discharged, would be helpful even now 21 months into my ongoing treatment.”
“There are too many moving parts within hospital departments and too many separate contacts to keep track of.”
“I was not advised of community resources available for cancer patients until after my treatment, and from sources other than my oncology team. I missed out on a lot of support that I could have had.”
Majority Would Embrace Digital Therapeutics Prescribed by Doctor but Many are Unsure
When asked whether they would use digital therapeutics prescribed by their doctor and made available to them, cancer patients and survivors were receptive to the idea by a ratio of four-and-a-half to one (63% likely to use versus 14% unlikely), however nearly a quarter (24%) say they are unsure.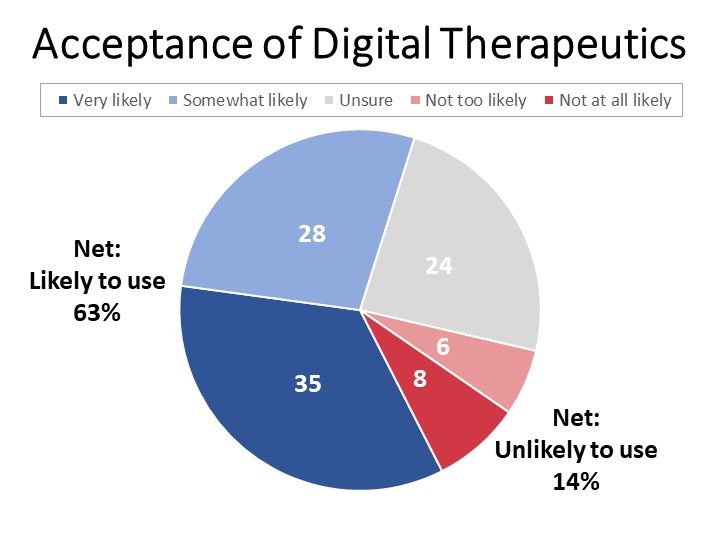
Digital therapeutics were defined in this survey as:
“…tools that deliver evidence-based medical interventions to patients via software programs to prevent, manage or treat diseases. For example, a cancer patient can report a cancer symptom or side effect of their treatment in an app and get personalized recommendations for managing it, while their care team can also monitor the patient remotely. Some digital therapeutics are approved or cleared by the FDA and can only be prescribed by a doctor."
Among the 14% who say they would be unlikely to use digital therapeutics, reasons for declining include concerns about costs (23%), that their needs are met without such a tool (11%), concerns about privacy (10%), and discomfort with technology (6%). These results suggest that clearly communicating the benefits of such a tool, any associated costs, and the protections in place to protect privacy would be essential to adoption and use.
Methodology:
ACS CAN’s Survivor Views research initiative was designed to enhance the organization’s mission to end suffering and death from cancer. Data provided by cancer patients and survivors as part of this project allows for a greater understanding of their experiences and opinions on cancer-related issues and gives voice to cancer patients and survivors in the shaping and advocating of public policies that help prevent, detect, and treat cancer and promote a more positive quality of life for those impacted.
To ensure the protection of all participants in this initiative all research protocols, questionnaires, and communications are reviewed by the Morehouse School of Medicine Institutional Review Board.
The survey population is comprised of individuals who meet the following criteria:
* Diagnosed with and/or treated for cancer within the last seven years
* Over the age of 18 (parents of childhood cancer survivors were invited to participate on behalf of their minor children)
* Reside in the US or US territories
Potential Survivor Views participants were invited to participate through email invitations, social media promotion, and partner group outreach. Those who agreed to participate after reviewing the informed consent information completed a brief survey including demographic and cancer history information to inform analysis as well as topical questions as discussed in this document. The data were collected between May 16-26, 2022. A total of 1,241 cohort participants responded to the survey, providing a margin of error of +/-2.8 percentage points at a 95% confidence level.
In addition to interviews conducted among the Survivor Views cohort, another 1,370 interviews were conducted among demographic groups that are often not included at sufficient numbers to allow for in-depth statistical analysis even when they are sampled at representative levels compared to the national cancer survivor population. This report summarizes the results of the cohort survey sample for consistency with other Survivor Views surveys, and includes the findings of our analysis of the oversamples where significant differences are observed among these groups.
The demographics of the cohort include:
• 16% Black/African American
• 9% Hispanic/Latino
• 3% Asian/Pacific Islander
• 17% Lower income households
The oversample interviews include:
• 589n Black/African American
• 497n Hispanic/Latino
• 229n Asian/Pacific Islander
• 524n Lower income households
About ACS CAN
The American Cancer Society Cancer Action Network (ACS CAN) is making cancer a top priority for public officials and candidates at the federal, state and local levels. ACS CAN empowers advocates across the country to make their voices heard and influence evidence-based public policy change as well as legislative and regulatory solutions that will reduce the cancer burden. As the American Cancer Society’s nonprofit, nonpartisan advocacy affiliate, ACS CAN is critical to the fight for a world without cancer. For more information, visit www.fightcancer.org.







